
What's inside My Health Record
Changes are being made to give you better and faster access to pathology and diagnostic imaging reports along with other key health information like immunisations, prescription and dispensing information, hospital discharge summaries and more, all in one place.

Getting started
Make sure you link Medicare in myGov first, for fast access to My Health Record. If you don’t already have a record, you can register for one at any time.

my health app
Download the my health app so you have all your electronic prescriptions and key health information in the palm of your hand.

Manage your record
You're always in control of your record. You can update your settings at any time, and decide what you'd like to store.

Privacy and access
How to manage access to your record.

Organisations
See which organisations are able to upload records.
The my health app
A secure and convenient way to keep all your electronic prescriptions and key health information in one place
Learn to use My Health Record
Register for upcoming online learning sessions or view recordings, including Auslan interpreted recordings.
We have an online learning module to help you understand more about My Health Record.
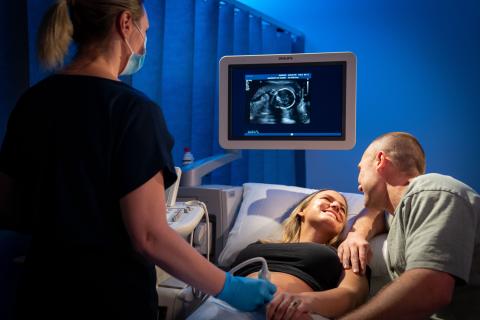
My Health Record for pregnant mums and newborns
Having your records in one place is invaluable when you have multiple care providers. Your record can help you and your healthcare providers keep track of your health information throughout your pregnancy and beyond.
You can also register your newborn for their record, so you can monitor their growth and development. It's just like a baby book, but instead of cute photos, there’s a picture of their health.
You can add the following to your child's record:
How to access My Health Record
Frequently asked questions
Digital health eLearning resources
Service availability:
There is currently no scheduled outage to the My Health Record system.

Search
Search for helpful information about My Health Record






